It's commonly believed that women should eat a lot more when they become pregnant. But that isn't true.
In reality, calorie requirements only increase by a relatively small amount during pregnancy. Often, just one extra snack per day is enough to meet calorie needs.
Pregnant women who start ‘eating for two’ run the risk of putting on excessive weight during pregnancy. Instead, women should aim to eat ‘twice as healthy’ and not ‘twice as much’.
A woman's total weight gain during pregnancy includes the mass of the fetus, placenta, amniotic fluid, increase in maternal body fluid and blood volume, fat stores and breast tissue that enables breastfeeding.
The appropriate amount of weight gain during pregnancy depends on a woman’s body weight and Body Mass Index (BMI) prior to pregnancy.
According to the Institute of Medicine (IOM), recommended guidelines for total weight gain during a full-term pregnancy are as follows:
Women who are underweight pre-pregnancy (BMI below 18.5), should gain 12.7 to 18kg.
Normal weight women (BMI between 18.5 to 24.9), should gain 11.3 to 15.8kg.
Overweight women (BMI between 25.0 to 29.9), should gain 6.8 to 11.3kg.
Obese women (BMI of 30.0 and higher), should gain 5 to 9kg.
Women gain only 5% of total pregnancy weight in the first 10–13 weeks of pregnancy. Most of the weight gain occurs in the second and third trimesters. The recommended rate of weight gain in the second and third trimesters are as follows:
For underweight women, a weight gain of 0.5kg per week.
For women with a normal pre‐pregnancy BMI, a weight gain of around 0.4kg per week during the second and third trimesters is recommended.
For overweight women, 0.3kg per week is recommended.
Gaining the recommended amount of pregnancy weight will decrease the chances of pregnancy complications, labour complications and the chances of having a high or low birth weight baby.
Babies born with a low or high birth weight (<2.5kg or >4.5kg) have an increased risk of abnormal development as well as various diseases in adulthood, such as heart disease, lung conditions, high blood pressure and diabetes.
Underweight women are encouraged to gain a minimum amount of weight to avoid low birth weight for the baby. In addition, underweight women who do not gain enough pregnancy weight are less likely to initiate breastfeeding.
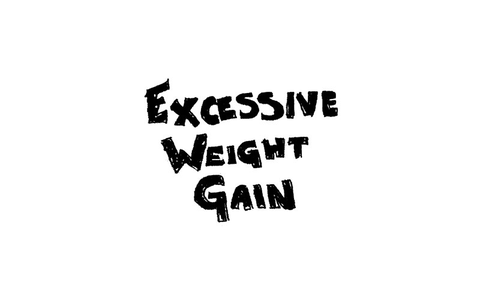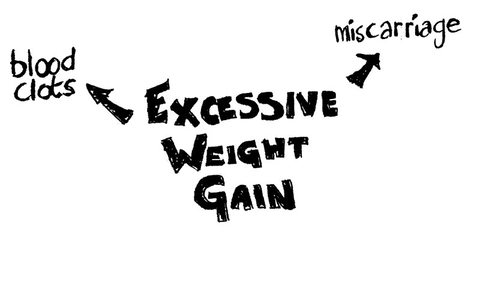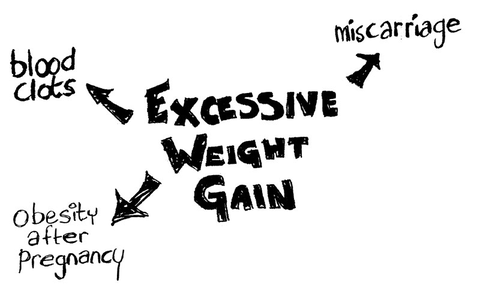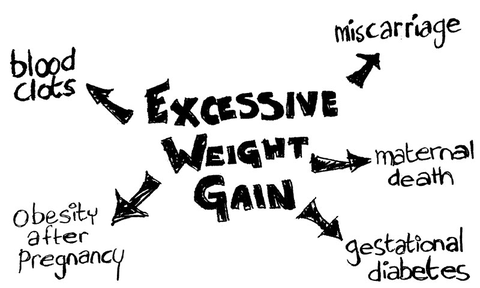
In contrast, excessive weight gain should be avoided. Women who are obese, or who put on too much weight during pregnancy have a higher risk of complications. These include gestational diabetes, miscarriage, pre-eclampsia, thromboembolism (blood clots) and maternal death.
The risk of labour complications and the risk of an emergency caesarean are also higher. In addition, a baby born to an obese mother is at increased risk of stillbirth, congenital abnormality and subsequent childhood and adulthood obesity.
Excessive weight gain during pregnancy may also cause the mother to become overweight and obese after childbirth. Based on many years of observational data, women who gain more than the recommended amount of weight during pregnancy tend to retain excess weight for up to three years post-partum.
Overweight women are advised to lose weight when they are trying to get pregnant, but once they have conceived, they should not diet to lose weight. This is because an insufficient energy and nutrient intake may have negative effects on the growth and development of the fetus. Instead, overweight women are advised to manage their body weight and follow pregnancy weight gain guidelines. They can do this by eating a healthy, balanced diet and taking part in regular physical activity.
This article is part of a series about pregnancy and nutrition. Check out the first instalment here.
All illustrations by Munnazzah Raza